When Kate Fitzgerald discovered she was pregnant with her first child in June 2020, she was elated that, at 37, she and her partner,
Lachlan, were going to be parents.
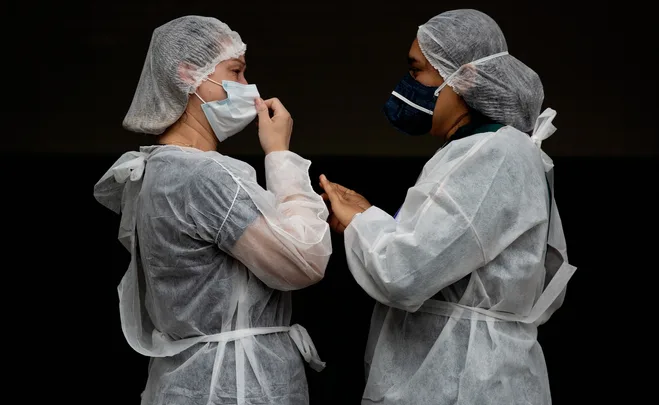
But like so many Australians, for Fitzgerald, the chief executive and deputy secretary of Emergency
Management Victoria, that elation was tinged with anxiety thanks to the complex overlay of the Covid-19 pandemic.
Check-ups were conducted via telehealth or not at all. Support was limited, as much of her family was trapped over the border in New South Wales.
“It was exciting – there was this pure joy of being pregnant,” she says. But when things began to go wrong, it became very, very difficult.
Fitzgerald began experiencing unusual symptoms – severe constipation, blood in her stools, extreme fatigue – about two months into her pregnancy. She had a suspicion something wasn’t right, yet she struggled to access adequate medical attention.
“Gastroenterologist and GP appointments were all telehealth,” she says. “And everything was dismissed as pregnancy related.”
In fact, after being passed from health professional to health professional, her symptoms became so pronounced she took herself to the emergency department of her local hospital. It turned out Fitzgerald had a tumour the size of a baseball in her bowel – stage two bowel cancer – and needed immediate surgery to save not only her own life, but that of her baby.
Incredibly, both Fitzgerald and her baby girl, Ava – who’s now more than a year old – survived the operation. (Miraculously, Ava was taken from Fitzgerald’s womb and kept alive for the duration of the surgery and then replaced to continue the pregnancy.) Fitzgerald has now been in remission for 21 months, but says the chaos of Covid caused her to suffer without a diagnosis for far longer than she should have.
“My diagnosis was delayed for at least two months as a result of not being able to access primary care in the way you ordinarily would,” she says.
“With telehealth, there was also this onus on me, the patient, to describe in a very medical way what I was feeling and what my symptoms were. No-one could physically examine me or really get a sense of my pain. And now I know that a delay of even a month with bowel cancer can increase your likelihood of dying by up to 10 per cent. That scares me. I had a two-month delay for no reason except Covid.”
Fitzgerald is one of thousands of Australians whose broader health was put on the back-burner because of a healthcare system that appeared to prioritise Covid over other health challenges. All over the country, people either struggled to access adequate healthcare, or were forced to access it by telehealth, which means nuance and context can be overlooked.
Then, others delayed critical screenings and other appointments because anything that wasn’t connected to Covid fell down their priority list.
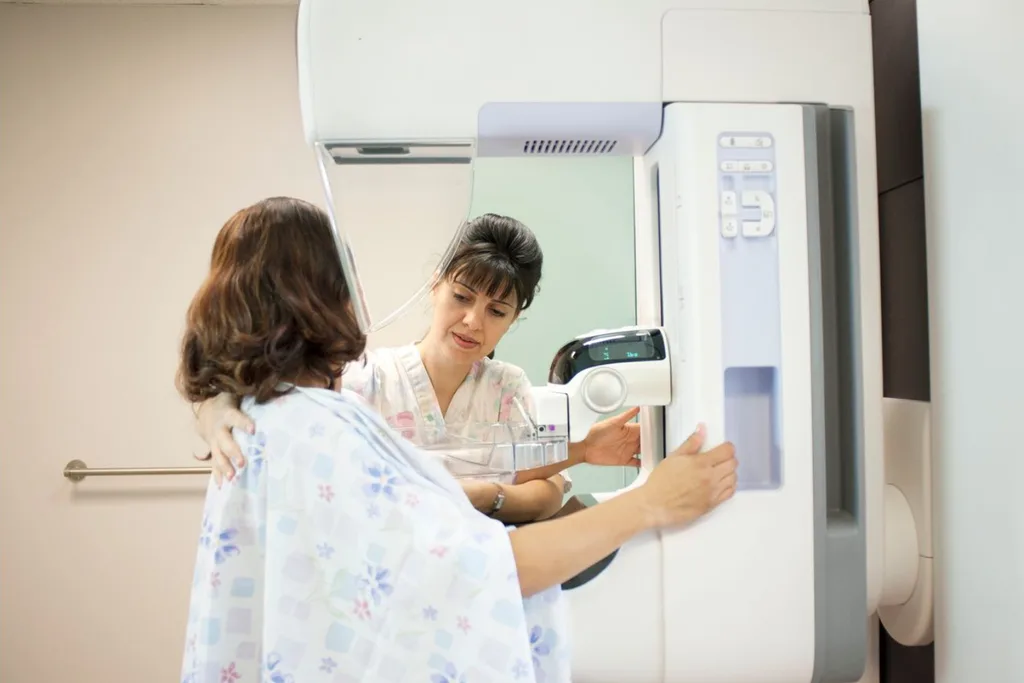
According to Cancer Australia, 164,000 fewer cancer diagnostic procedures – such as mammograms and colonoscopies – happened in 2020 than in an ordinary year. Pathology numbers – such as blood tests and biopsies – also plummeted.
In April 2020, one of Australia’s largest pathology providers, Clinical Labs, saw their normal numbers fall by 40 per cent. Between January and October 2020, the clinic found that their Victorian labs recorded a reduction of 17 per cent in malignancy diagnoses, and the numbers were similar in NSW.
The results of these delays aren’t necessarily being seen yet – Cancer Australia estimates that up to 20,000 missed cancers could surface in the next few years – although the statistics trickling in are already causing huge concern among health professionals.
Bowel Cancer Australia says that in 2020 there were 376 fewer surgeries than in 2019 (pre-Covid).
In 2021, those numbers surged, with 120 more bowel cancer surgeries performed compared with 2019. At the height of the pandemic there was a massive drop in colonoscopies of 57 per cent. The suggestion is clear: that the huge decline in screenings during Covid –87,000 fewer in 2020 compared with 2019 – is beginning to show up in the form of advanced cancers.
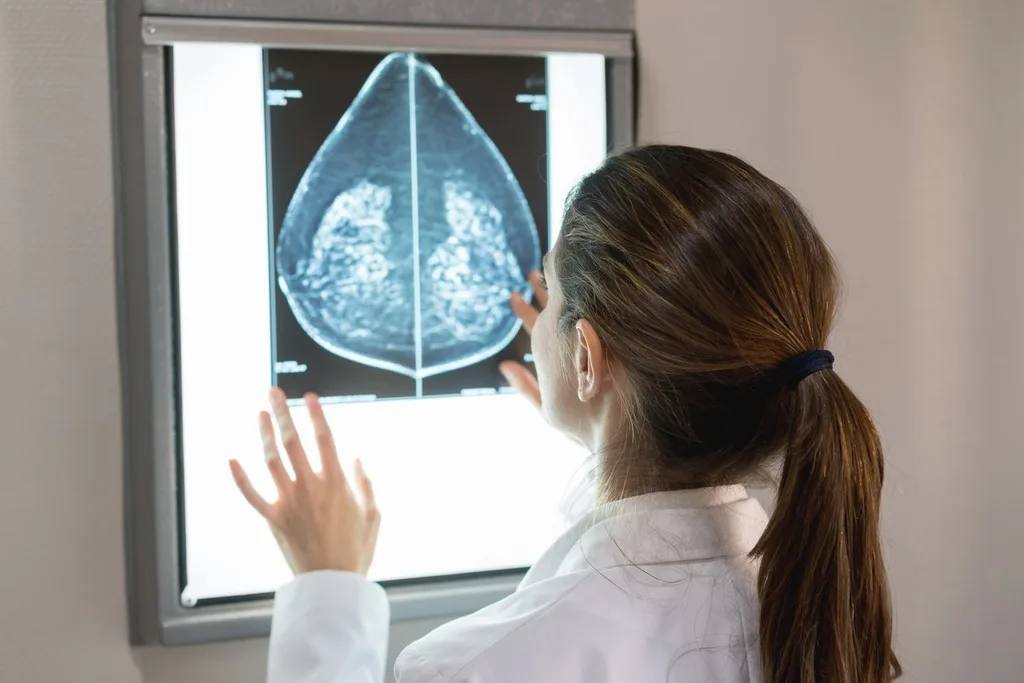
“We tried to get campaigns out there to remind the community that cancer doesn’t wait,” says Kirsten Pilatti, CEO of Breast Cancer Network Australia (BCNA), whose members also reported that both screening and diagnosis for breast cancer plummeted all around the country.
“We knew Covid hadn’t cured cancer. But we could see that people were afraid to go out, or didn’t want to burden the healthcare system. Particularly with women, they tend to prioritise everyone else and deprioritise themselves. So they’d … stop being proactive about their health.”
Melbourne mother-of-three Nicole Armstrong, 54, fell squarely into that category. As an immune-suppressed heart-transplant recipient she felt particularly vulnerable about exposing herself to Covid by going out into the community. She was also busy making sure everyone else in her family was taking care of themselves throughout the pandemic – a common story with women.
“I had been due for a mammogram in 2019, and I’d said to myself yes, yes, I’ll do it,” Armstrong recalls. Her own mother – a breast cancer survivor – had also been “on her back” about her checks, but something had always come up.
“Then Covid hit in 2020. Subconsciously I think I thought, ‘Oh, everything’s online. No-one’s really seeing doctors. I’ll do it eventually. But not right now’.”
It wasn’t until August 2021 that she received a sudden, terrifying, reminder. “I leant across a bench and felt a sore bit in my breast, and I thought ‘no, that’s not right’,” she recalls.
She went to her GP and that afternoon had a mammogram and ultrasound. “I think I just knew,” she remembers. “When you know you know.”
After three weeks of appointments and tests, Armstrong was diagnosed with a large triple-negative tumour in her right breast. Within days she was booked in for a full mastectomy, followed by four rounds of chemotherapy. Today her prognosis is fairly positive.
“I think I’m very lucky they got it when they did,” Armstrong says. “It’s a very aggressive, fast-growing cancer. Maybe if I’d had the screening in 2020 it would have been smaller. Of course, I did wonder over and over: maybe if I’d done the check when Mum reminded me, maybe it was sitting there, maybe they could have caught it sooner. Let’s put it this way – I’m glad
I didn’t delay any further.”
Medical oncologist and clinician scientist Dr Belinda Yeo, who works at Melbourne’s Austin Hospital and Olivia Newton-John Cancer Research Institute, suspects stories like Armstrong’s will become increasingly common in the next few years, both among people who missed routine screenings and turned out to have asymptomatic cancer, as well as those who actually discovered breast cancer symptoms during lockdowns.
“Our assumption is that patients who had a lump or other breast complaint [during the pandemic] would have sought medical care, but we know that’s not necessarily the case,” she says. “Even those people put investigations off, because we put off so many things.”

Her concern is not just for the women who missed critical screenings during the height of the lockdowns, but also those who still haven’t begun to reprioritise their health now that the country has reopened.
“We know that fewer cancers were diagnosed across the pandemic but I suspect this is actually continuing,” Yeo says. “We’re not through this yet. There are plenty of people who are feeling pretty vulnerable or who – now that the pandemic feels like it’s quieting down – aren’t thinking about their breast screen. They’re thinking about going on holiday.”
And that, she says, could really begin to show up in the next few years. “I think it will take years for us to learn what the impacts have been,” Yeo says.
“For the cancers that we do diagnose over the next few years, we can only hope that their treatment won’t have to be more intense but a proportion absolutely will be.”
The BCNA’s Kirsten Pilatti says, “The people who didn’t get checked and go on to have cancer, we’ve just got to hope we find it as early as possible. We know that if we find a cancer early, we can treat it early and work towards that person being cancer-free. But the challenge is the longer you wait, particularly with breast cancer, the higher the risk of it going on and metastasising throughout the rest of the body where it’s incurable.”
Those seeking treatment for existing cancers and other conditions aren’t out of the woods, either. All over the country, healthcare services are struggling to function under a Covid burdened system, whether it’s through crowded emergency departments, staff
shortages or dealing with the backlog of medical issues that weren’t treated during the pandemic.
All of this is placing yet more stress on cancer patients. Pilatti reports that women waiting for post-mastectomy breast reconstructions are sitting on long waiting lists with no indication of when they might be prioritised, something she says adds an extra layer of emotional distress.
Another patient, Monique Henderson, told marie claire she was forced to miss a round of her three-weekly infusion treatment for
metastatic breast cancer because she contracted Covid this year and had to isolate.
“If my cancer recurs I’ll never know if it’s because I skipped that round of treatment,” she says. “I guess it’s just a matter of … fingers crossed.”
The question has to be asked: did governments and health bodies correctly weigh the prioritisation of Covid-19 against other health issues? And not just on the health side; did we get the compassion right too? Thinking back to those people who were forced to say goodbye to loved ones in palliative care via Zoom, or face a lonely operation or other major challenge without family support, was that the right thing to do? It’s impossible to say – yet. Undoubtedly, this period of time will be retrospectively studied for generations to see how we could have done better.
Kate Fitzgerald, now a Bowel Cancer Australia ambassador, has the interesting perspective of both sides, having suffered through the enormity of bowel cancer and pregnancy during the height of the pandemic, and as someone who works in the healthcare system.
“I do understand why decisions were made to free up the healthcare system and focus on Covid,” she says.
“People were dying and the numbers were significant, particularly here in Victoria. And messaging around things like vaccinations were also really important to prioritise. But if we were to go through another wave of Covid, I think we would need to look at a more risk-based approach to things like telehealth. And make sure that the message gets out there that other health issues simply do not stop.”
In 2021, the then-NSW premier Gladys Berejiklian coined the phrase “there’s no perfection during a pandemic”. But should we face a similar global health crisis again, many health professionals would like to see a more holistic approach to our existing health challenges, which do not go away just because a new one has appeared.
“I wish we’d seen more nuance in the message,” adds Pilatti. “[For example] stay home. But if there’s something you’re worried about, continue to seek support.”
This article originally appeared in the August issue of marie claire.